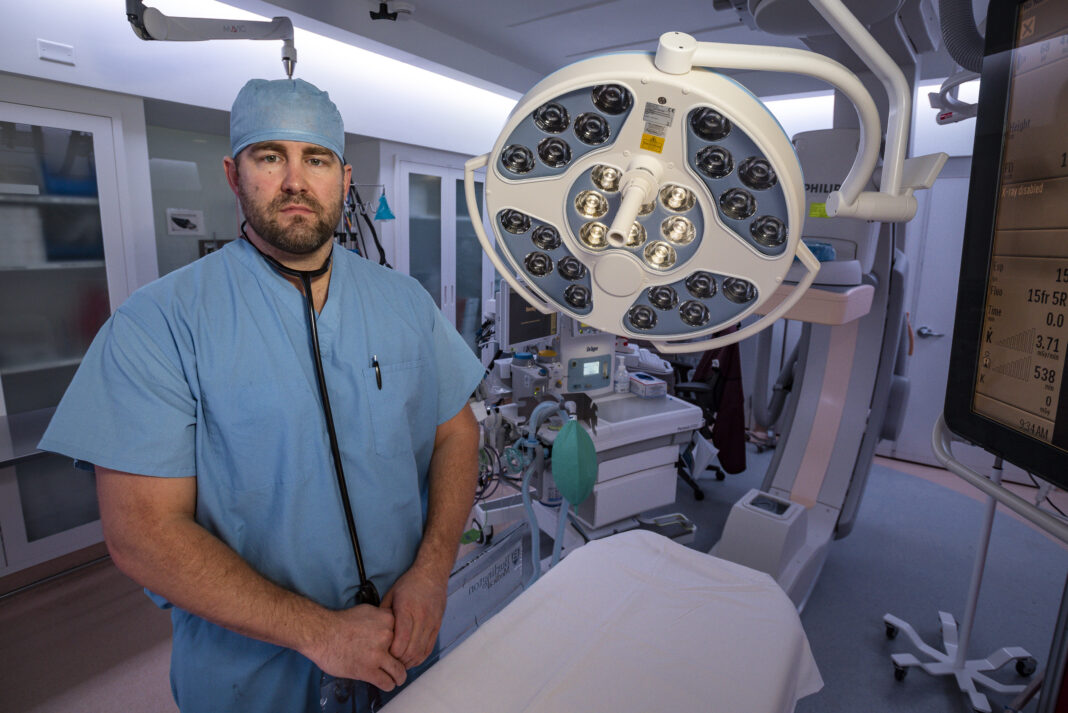
Since 2019, cardiologist Dr. Adam Farber has been providing the minimally invasive transcatheter aortic valve replacement, or TAVR procedure at Medical Center Hospital.
TAVR is also called TAVI, or transcatheter aortic valve implementation.
“It’s a procedure used to treat aortic stenosis, which is a valve disease and one of the main valves of the heart, when the valve becomes too stiff, and it’s calcified it does not open correctly. Sometimes it leaks too much, as well. Your heart is a pump and has to pump the fluid through this valve. When the valve doesn’t work right, the heart can become very weak. Unfortunately, for patients who have this, the prognosis becomes poor rather quickly, especially once the heart becomes weak, or they develop symptoms. … Typically we say within two years, about half of people are at risk of dying, so it’s going to be rather progressive. …,” Farber said.
He added that a lot of people have aortic stenosis, but not a lot of them have severe aortic stenosis that need a valve to be treated.
Probably close to 1 percent of the population will eventually have this.
“It’s something that is definitely associated with age and (it) changes with age. But there are some pathologic conditions with the valve. People are born with an abnormal valve sometimes, and when you have that those valves calcified early in life, as early as 50s or 60s sometimes. This kind of procedure is used to treat those valves without having to cut the chest,” Farber said.
Some people do fine with open heart surgery to replace a valve, but particularly older patients who have multiple comorbidities such as lung disease or other reasons that you would not want to open their chest, we would expect to not heal well after an open heart surgery.”
“This provides an excellent potential alternative. … Usually we go in through the arteries in the legs, implant the valve and in the next day they go home. Actually now, for most of these procedures, we don’t even put the patient to sleep. We sedate them a little bit with medication, but they’re breathing on their own. They’re not even on a breathing machine. It’s really quite minimally invasive and so it’s really been beneficial,” Farber said.
The hospital has performed 47 of the procedures since fall 2019.
The valve is replaced with a valve prosthesis.
“Depending on which company you use, that material may be made from two different animals porcine or bovine, a pig or cow. That tissue is actually sewn into a 3-D structure that simulates valves. And it’s actually within a metal structure that we call it a frame or a stent. We are able to employ that and that metal frame sets up a scaffold, and then the leaflets that are sewn in a special way. They function as a one-way valve, essentially,” Farber said.
“Typically these kind of bioprosthetic valves which have been implanted surgically before, 10 to 15 years for most of them; okay, some of them a little shorter; some of the little longer … so we’re expecting that kind of range. Our data so far looks like that’s going to be what we expect …,” Farber said.
The procedure started in Europe and it began in the U.S. several years later.
“… There’s definitely a patient population that we have treated for a long time before this valve was available here who do not want to travel places. Being able to provide that service here, I think, has been helpful for them because these are oftentimes very elderly, ill people and traveling … to places like Dallas and Houston can be rather challenging. Some of them will choose not to do that,” Farber said.
This also is a big deal for the region because there is an elderly population in the outlying areas that are hard to reach.
“… This is becoming a little more widely available as the techniques and the tools are refined …,” he said.
Dr. Mark Davis, an interventional cardiologist in Midland, also performs TAVRs.
“We started … collaborating, working on those together, and he’s doing those in Midland now,” Farber said.
He added that Dr. Kirit Patel, a surgeon, has to do the procedures with Farber and/or Davis.
“(It is) mandated that you have a surgeon in the room and this is really for patient safety that if you have an emergency, they’re able to actually go into the chest and fix it immediately. So it’s actually mandated that this is a two-operator procedure,” Farber added.
The actual time of the procedure is 30 to 45 minutes. A more difficult case can take longer, maybe an hour or two.
On average, they go home the next day.
“… For open heart surgery, the surgery itself is probably three to six hours, depending on how much other work needs to be done for just the surgery. And the patient’s on a ventilator sometimes for several days afterwards. Recovering from these can vary depending on the health of the person, three to five days on the short end; several weeks on the long end before you can get out of the hospital. But then after that the recovery, substantial cardiac rehab, sometimes older patients need inpatient rehab help, and then returning to a normal life is something that takes several months, for sure,” Farber said.
The holes they make in the leg arteries are what limits them the most. But once those heal, usually within one or two weeks, patients can go back to daily activities of living. However, Farber would not advise lifting anything heavy for a couple of weeks.
Louis Davitt of Fort Davis was brought by air ambulance to Medical Center after having a minor stroke. He was scheduled for the procedure in fall of last year after it was discovered that he needed a heart valve replacement.
“The procedure itself was a non-event as far as I was concerned. I checked into the hospital at 5 o’clock one morning and they did the procedure that morning and I checked out of the hospital the following afternoon. I was only in overnight,” Davitt said.
After the procedure, he said they found there was little or no damage to the heart itself other than the valve.
“Getting that fixed made a world of difference,” Davitt said.
He added that he now has no restrictions at all on what he can do.
“The actual TAVR procedure compared to the alternative that they used to do, have to crack you open and do open heart surgery to replace that valve. There’s no comparison. The only recovery I had was I couldn’t drive for the first week afterwards and no heavy activity for the next week,” Davitt said.
Two weeks after the surgery, he said he was clear to do anything he wanted.
“The surgeon, Dr. Farber there in Odessa, I got nothing but good things to say about him and his whole team really,” Davitt added.
This procedure and open heart surgery have been shown to prolong patients’ lives.
“… Our real question at this point, because both techniques are well refined, is which one’s going to serve the patient best … There are a lot of factors that go into that, the health of the patient, the durability of the valves, things like that. So this procedure, particularly in our older patients who are high risk, for sure lengthens life compared to open heart surgery,” Farber said.
Signs and symptoms of aortic stenosis, initially for most people, are shortness of breath, or chest pain, which would be tightness, heaviness or squeezing.
Farber said some patients say they are having discomfort.
Some of the signs may be climbing stairs or something with a higher level of exertion.
“But the valve changes very slowly over many years, so a lot of people just slow down and they don’t develop a real sudden change in symptoms. … Swelling in the legs and difficulty breathing or when they’re laying down are the typical signs,” Farber said.
“One sign that we have been really worried about is sometimes people pass out from this. It can be a reason people are losing consciousness and that one is particularly worrisome. (It) is usually indicative of fairly advanced disease,” he said.
If the valve is the only problem, Farber said they can fix it and a lot of times they are fixing them in 80 and 90 year olds.
For someone to live that long, he said, they usually live a fairly healthy lifestyle.
He added that those with blocked arteries, for example, they are cautioned to live a healthier lifestyle.
Farber said they can put a valve inside a young person and they can put a valve inside a valve years later. But you can’t take it out without opening up the chest.”… And so we will find out that answer in the years to come …,” he said.
Farber said the valves can degenerate and sometimes they can malfunction, but that is very rare.
He added that he wished to express gratitude to Dr. Patel and Lissette Aguirre, who is their valve coordinator.
“Those two have been instrumental in starting the program here” and they couldn’t have done it without those two, Farber said.